It's time to shrink your bubble
More Americans are getting sick right now than ever before in the course of the pandemic. Here's how you can conceptualize the big numbers and what you can do to help.
Welcome back to the COVID-19 Data Dispatch.
I don’t have a pithy introduction this week because the numbers are truly terrifying. More Americans are getting sick right now than ever before in the course of the pandemic, and within weeks, more Americans will be dead than we know how to memorialize.
This week’s issue walks through those numbers and how we can respond. I’m also taking a data perspective on the Pfizer vaccine news and President-Elect Biden’s transition, and sharing the results of last week’s reader survey.
National numbers
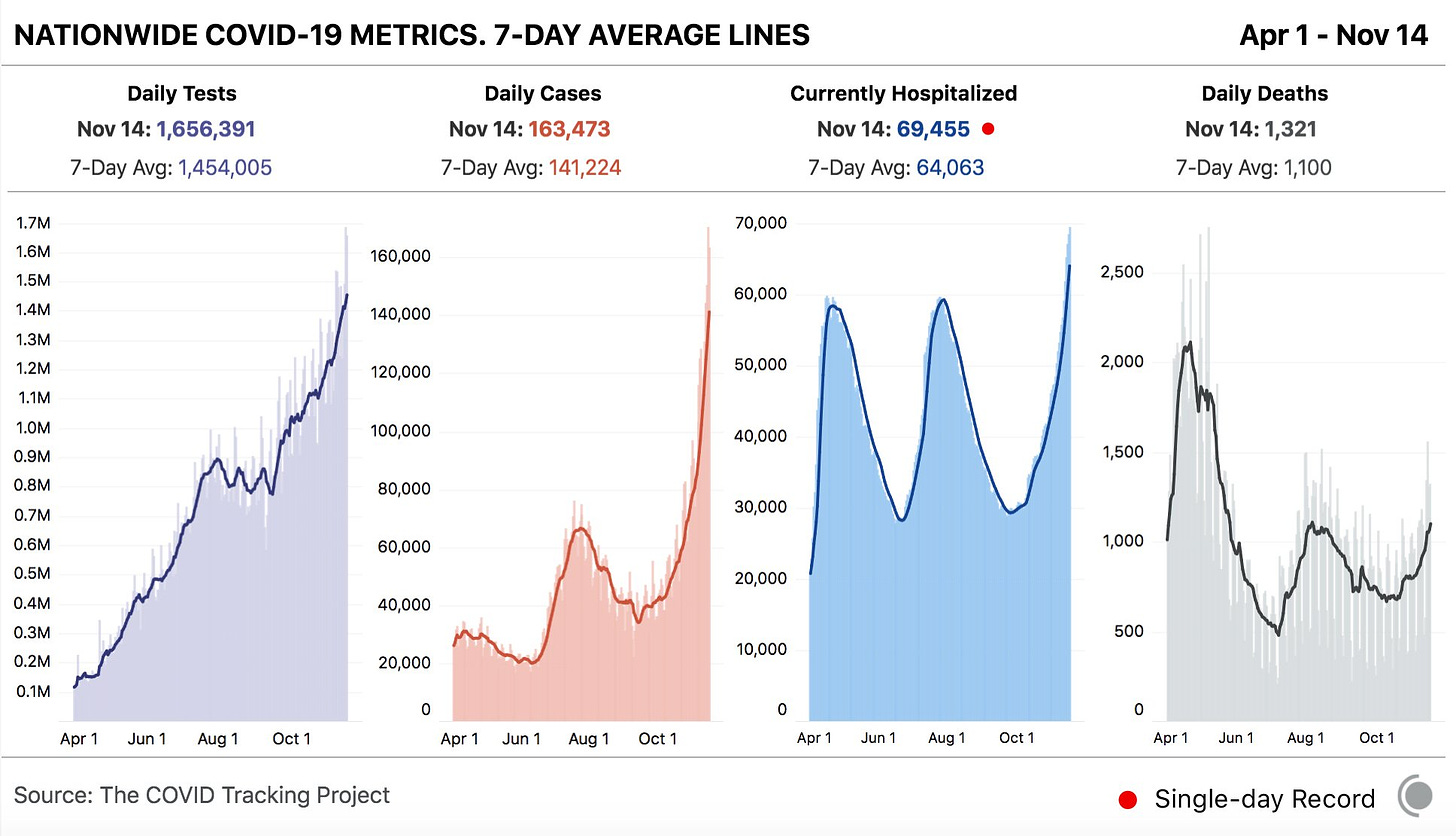
In the past week (November 8 through 14), the U.S. reported about 990,000 cases, according to the COVID Tracking Project. This amounts to:
An average of 141,000 new cases each day (38% increase from the previous week)
302 total new cases per 100,000 people
1 in 331 Americans getting diagnosed with COVID-19
3.4 times the total cases Canada has reported over the entire course of the pandemic
Cases continue to rise across the country; 38 states reported over 1,000 cases yesterday. The COVID Exit Strategy tracker now categorizes every state except for three as “uncontrolled spread,” and even Maine and Vermont are now “trending poorly.”
America also saw:
7,700 new COVID-19 deaths last week (2.4 per 100,000 people)
69,000 people currently hospitalized with the disease, as of yesterday (24% increase from the previous week)
So many people have been infected and become seriously ill in recent weeks that hospital systems are overwhelmed. Two new articles published this past Friday, by ProPublica’s Caroline Chen and The Atlantic’s Ed Yong, center the experiences of America’s stressed, scared, and exhausted healthcare workers. Both pieces give faces and voices to these immense numbers. If you read nothing else this weekend—even if you don’t read the rest of this newsletter—please read those two stories.
I offered my own take on the current outbreak in a Twitter thread last Wednesday. This is the message I want to highlight:

We already know what we need to do to get this nationwide outbreak under control. We did it in March. Stay home. Limit your activity and travel to the essentials. Shrink your circle of contacts. Take care of your neighbors. And, whenever you’re outside the house—wear a mask.
A new metric for conceptualizing cases
Last week, a new metric appeared in the COVID Tracking Project’s daily updates. Within days, this metric was also featured in my newsletter, Benjy Renton’s Off the Silk Road, New York Governor Andrew Cuomo’s Twitter account, NPR, and even the New York Times.
Here’s how it works. You take the number of COVID-19 cases reported in the past week and divide the current U.S. population by that case number. There are variations; the metric may also be calculated for different time spans or smaller geographies, such as a specific U.S. state. But the standard calculation focuses on the nation, over the past week.
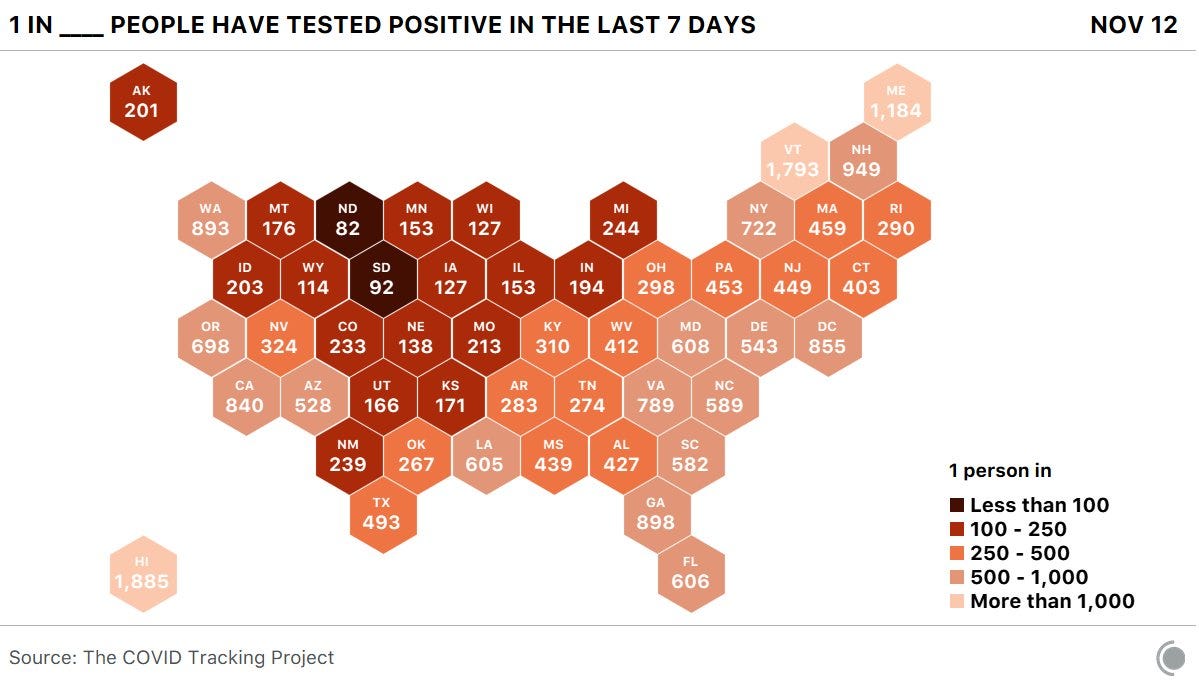
For example: in the past week, one in 331 Americans has been diagnosed with COVID-19. If we extend that out to the past two weeks: one in 192 Americans has been diagnosed with COVID-19 since November 1.
Here’s what it looks like by state (reflecting data from November 5 to 12):
The biggest challenge that data journalists like me face right now is putting massive COVID-19 numbers into a context that readers may easily understand. I’ve used a variety of analogies, comparisons, and visualizations, but I like this number because it feels visceral. I’ve had lectures smaller than 331 people. I’ve been to protests ten times bigger. It’s a number of people that I can picture, a number of people that would fit in my neighborhood park.
Among COVID Tracking Project volunteers, this metric is known as the Camberg Number—after Nicki Camberg, City Data Manager at the Project, who first shared it in Slack earlier in November. I asked her where she got the idea for this calculation and how she’s thinking about pandemic data during this terrifying surge.
Here’s what she said:
When thinking about COVID-19, the metrics we’ve been using have started to blur together and stop having the same impact after months of staring at them. What is the difference between 100,000 and 150,000 new cases? Well, obviously, 50,000 more cases, but I can’t conceptualize that, nor can most people. Numbers that high feel almost abstract and easy to ignore. I could feel myself starting to normalize these increasing case and hospitalization rates, and I had to figure out a way to stop that from happening. If I, someone who spends all day every day collecting, discussing, and working with COVID-19 data, was starting to get desensitized to the pandemic—what must it be like for the general public?
I knew I had to find a way to make it more personally relatable, but also find a way to use the data I look at every day to better inform my own decisions. When I go to the grocery store, what is the probability that someone in the store with me tested positive? How many people in my grade currently have COVID? If my grandmother leaves her house, how many people does she have to interact with before it’s likely she was in the presence with someone who could infect her?
The first time I calculated this number was November 5th. The US had just hit 116,000 new cases in a day, the second day in a row of record breaking cases and the start of a week of near-constant exponential increases. I calculated that roughly 1 in 3,000 Americans were diagnosed with COVID-19 that day, and I was shocked. 1 in 3,000 people? That number felt like a punch in the gut, and made me see the devastating effect of this pandemic more than any other statistic I’d heard for months. It gets even worse when this is applied to state or local levels (which one can do using the newly released CTP City Dataset), and it is genuinely devastating when done by race.
From the feedback I’ve gotten, it seems like a lot of people are feeling the same way I am: jaded and exhausted after half a year of a never ending pandemic. Sometimes we need a shock to the system to realize that this is not normal, is not something that can be ignored. Until there is a vaccine, cases will only continue to spike with the holiday season unless we all choose to practice radical empathy and collectively do all we can to curb the spread of the virus.
Questions? Comments? Leave a public note on the post, or hit me up at betsyladyzhets@gmail.com.
How to think about vaccine results
This past Monday, pharmaceutical company Pfizer announced preliminary clinical trial results for its COVID-19 vaccine. In an interim analysis of the vaccine’s phase 3 study, the vaccine was shown to be 90% effective in preventing COVID-19. In other words, based on the people in Pfizer’s study who have become diagnosed with COVID-19 so far, those who got vaccinated were 90% less likely to get sick compared with the people who did not.
90% is an exciting number. The Food & Drug Administration (FDA) set a threshold of 50% effectiveness for COVID-19 vaccines to be authorized, and experts have been telling us for months that even a 60% or 70% effectiveness would still be incredibly useful in reducing infections across the population. Pfizer’s initial 90% rate blows those expectations out of the water.
Plus, this effectiveness value bodes well for other vaccine candidates. Pfizer’s vaccine, developed through a partnership with German biotech BioNTech, uses a new vaccine technology based on synthetic messenger RNA, or mRNA; so does the vaccine developed by Moderna, which is also currently in clinical trials. (For more backstory on mRNA, BioNTech, and Moderna, I highly recommend Damian Garde’s feature in STAT News.)
But we can’t get too excited. Pfizer reported its preliminary data not in a peer-reviewed scientific paper, but in a press release, and some key details about the company’s clinical trial are not yet public. I used information from STAT News, KHN, and SciLine to compile a few key questions that should be in all of our minds as we think about this and future vaccine data releases.
What is the sample size? Or, how many people were involved in the trial, and how many of them were diagnosed with COVID-19? For Pfizer’s trial, this is a question we can answer: about 44,000 people are enrolled in the study, and the 90% effectiveness rate is based on results from 94 people who contracted COVID-19, the majority of whom did not receive a vaccine dose. This may seem like a tiny fraction of the participants, but many experts are cautiously optimistic in hoping the 90% rate will hold up for a larger group.
Who is included in the sample size? COVID-19 has disproportionately impacted the elderly, people of color, people with certain medical conditions, and other marginalized groups. It is thus crucial that a vaccine is effective for people in these groups—in other words, these people must be represented in the vaccine trial. Pfizer reports that 42% of the overall study participants have “diverse backgrounds,” but the specific backgrounds of the patients who got sick are unknown.
Does the vaccine work for severe cases? While the majority of people diagnosed with COVID-19 are able to survive the disease with mild symptoms in their own homes, the minority of people who become seriously ill constitute the pandemic’s massive loss, as well as its burden on our nation’s healthcare system. A vaccine that reduces the disease’s severity through boosting immune system defenses may be incredibly valuable, even if it does not entirely prevent infection.
Does the vaccine work for mild or asymptomatic cases? A vaccine that prevents mild cases would help keep COVID-19 spread at bay, even if this vaccine does not reduce the disease’s severity. Pfizer’s press release does not include any specifics on the 94 patients who were diagnosed with COVID-19; experts are hoping that such details may be revealed in a forthcoming scientific paper.
Does the vaccine have any adverse effects? In other words, is the vaccine safe? We all know that flu vaccines make our arms sore, and other vaccines can give us mild colds. These types of common effects are usually nothing to worry about, but vaccines may pose a more severe danger to a small fraction of the population; for example, one in every ten thousand patients might have an allergic reaction that sends them to the hospital. So far, Pfizer has not reported any severe effects of its vaccine, but the current clinical trial gives the company a much wider pool of people in which dangerous reactions might be observed.
What are the vaccine’s logistical needs? One dose or two? At what temperature does the vaccine need to be stored? How long can it be at room temperature before it needs to be administered? How many doses can be manufactured in a day, a week, a year? What’s the price tag? Pfizer has given preliminary answers to some of these questions (two doses, -70 degrees Celsius) but the company is finalizing its manufacturing and distribution strategies as it completes its clinical trial.
Even when a vaccine is authorized by the FDA, distributing and tracking it poses a whole new set of questions. I’ve written about vaccine data before, and I expect that this will be a topic I cover in increasing detail during the months to come.
What a President Biden could mean for COVID-19 data
Last weekend, President-Elect Biden and Vice President-Elect Harris unveiled a Transition Plan. Their website covers detailed steps that the new administration intends to take for addressing COVID-19, climate change, economic recovery, and more.
One item in the COVID-19 plan caught my attention immediately:
Create the Nationwide Pandemic Dashboard that Americans can check in real-time to help them gauge whether local transmission is actively occurring in their ZIP codes. This information is critical to helping all individuals, but especially older Americans and others at high risk, understand what level of precaution to take.
A nationwide pandemic dashboard? Standardizing information from all 50 states? Providing local data down to the ZIP code level? This is literally all I’ve wanted from federal COVID-19 data since February. If the Biden team provides a publish date for this dashboard, I will mark it on my calendar and eagerly count down the days.
But, as you might imagine from reading my Source Callouts, I have a lot of thoughts on what types of organization, design, and documentation can make COVID-19 dashboards either easy to use—or frustratingly complex. Many other COVID Tracking Project volunteers, who have similarly been wading through state dashboards, have similar expertise. A group of data entry veterans, designers, science communication specialists, and other Project volunteers put together a set of recommendations for the dashboard that President-Elect Biden’s administration might build.
You can read all the recommendations on the Project’s blog. Here are a few highlights:
Prioritize clarity, by putting the most important data points front and center.
Offer transparency, through accessible data definitions and methodologies as well as time series which allow users to see how metrics have changed over time.
Structure the dashboard with consistency, through the use of logical section headers, color schemes, and regular updates.
Provide absolute and per capita values for all major metrics.
Report different test types seperately, and provide both positives and totals to allow for accurate test positivity calculations.
Make the design inclusive, through providing access for different internet connection speeds, mobile use, and easily surfaced information (i.e. no hovering).
Provide annotations and disclaimers to help users understand caveats and complexities in the data.
Include data in the forms of charts, sortable tables, and downloadable spreadsheets to allow for easy analysis.
Place sex, age, race/ethnicity, and other demographic data in context by comparing COVID-19 rates with the overall population.
There’s a pretty big caveat to my dashboard excitement, though. In order for President-Elect Biden’s administration to put together a Nationwide Pandemic Dashboard, his team must first be able to access the nationwide pandemic data. So far, as President Trump has yet to concede the election, current Department of Health and Human Services (HHS) leadership are not able to communicate with their successors. POLITICO’S Adam Cancryn described the situation in a November 10 story:
Biden’s HHS transition team is not yet allowed to have any contact with its agencies, including with officials at the center of the pandemic response like infectious disease expert Anthony Fauci and HHS testing czar Brett Giroir. It’s also barred from accessing nonpublic information or setting up government offices, limiting the new administration’s ability to get a full picture of the public health crisis that it’ll take responsibility for in just over two months.
The separate coronavirus-specific squad has been held up as well, over concerns about how to structure it ahead of the formal start of the transition process and how willing the Trump administration will be to cooperate.
The sooner top national politicians accept the election results, the sooner Biden’s COVID-19 team can get to work. That work includes data dashboards, ramping up testing, public health communication, and just about everything else we need to get the virus under control.
This newsletter is a labor of love for me each week. If you appreciate the news and resources, I’d appreciate a tip:
Our favorite COVID-19 sources
Last week, I asked readers to share their go-to sources for COVID-19 data about their community. Thank you to everyone who responded! I am always on the lookout for great sources myself, so I appreciated seeing what folks are using.
Here are a couple of responses that I wanted to highlight:
The New York Times cases map: Two readers noted that they liked the NYT dashboard, which makes it easy to compare COVID-19 metrics in different parts of the country. The NYT offers data at the county level and provides annotations and context with much more detail than most government sources.
City and county sites: Seven readers said that they regularly check their county or city dashboards for local information. One reader complimented the City of Chicago dashboard as “consistently updated with official data, easy to use.”
Social media: Readers referred to Twitter links to articles shared by both national and local journalists. One reader praised daily COVID-19 update posts shared on a local Boston subreddit: “The posts take publicly available Massachusetts health data and synthesize them in a way I've gotten very used to. This is the source I depend on when I tell people that COVID hasn't been getting better in Massachusetts since June.”
The Glastonbury Town Manager weekly email: My mom’s favorite source is the email newsletter sent by the local administration in my hometown, Glastonbury, Connecticut. This email—which I’ve highlighted in the newsletter before—includes data for the town, updates for the state, and public service announcements.
New York Governor Cuomo’s daily updates: You have to hand it to him: no other local leader is using PowerPoint quite like Cuomo. Also, nobody else built a literal model of his state’s COVID-19 case curve.
Please keep an eye out for our next survey, coming straight to your inbox next Sunday.
Featured sources
These sources, along with all others featured in previous weeks, are included in the COVID-19 Data Dispatch resource list.
The COVID Tracking Project’s City Dataset: For about five months, COVID Tracking Project volunteers collected and standardized data from highly populated cities and counties across the country. The project started in late May with the intent of tracking COVID-19 in cities that were seeing large Black Lives Matter protests, then expanded following the Sunbelt surge in June. 65 cities and counties are included in the dataset; you can read more about the dataset’s methodology and major findings on the Project’s blog.
COVID-19 State and County Policy Orders: This dataset includes over 3,000 COVID-19-related policies at the state and county level addressing public health, local economies, and disparities during the pandemic. Data were compiled by students at the Boston University School of Public Health and other student volunteers, and the dataset is housed at the HHS.
School outbreaks in Maryland: Maryland has become the most recent state to report school COVID-19 data, including total cases associated with every K-12 school in the state. Neither testing numbers nor enrollment numbers are available, making it difficult to contextualize these case counts.
More recommended reading
My recent bylines
Worried About Getting a Flu Shot This Year? Medical Experts Answer Your Top 20 Questions (Healthline)
From Wuhan to the White House: A timeline of COVID-19’s spread (Stacker; updated 11/10)
News from the COVID Tracking Project
Bonus
Making a School Reopening Decision and Taking the Heat (Education Week)
Nursing Homes Still See Dangerously Long Waits for COVID Test Results (KHN)
That’s all for today! I’ll be back next week with more data news.
If you’d like to share this newsletter further, you can do so here: